Impact Factor
Theranostics 2014; 4(9):893-903. doi:10.7150/thno.9425 This issue Cite
Research Paper
An EGFR Targeted PET Imaging Probe for the Detection of Colonic Adenocarcinomas in the Setting of Colitis
1. Athinoula A. Martinos Center for Biomedical Imaging, Department of Radiology, Massachusetts General Hospital, Harvard Medical School, Boston, MA;
2. Department of Medicine/Division of Genetics, Brigham and Women's Hospital, Harvard Medical School, Boston, MA.
Received 2014-4-17; Accepted 2014-6-4; Published 2014-7-1
Abstract
Colorectal cancer is a serious complication associated with inflammatory bowel disease, often indistinguishable by screening with conventional FDG PET probes. We have developed an alternative EGFR-targeted PET imaging probe that may be used to overcome this difficulty, and successfully assessed its utility for neoplastic lesion detection in preclinical models. Cetuximab F(ab′)2 fragments were enzymatically generated, purified, and DOTA-conjugated. Radiolabeling was performed with 67Ga for cell based studies and 64Cu for in vivo imaging. Competitive binding studies were performed on CT26 cells to assess affinity (KD) and receptors per cell (Bmax). In vivo imaging using the EGFR targeted PET probe and 18F FDG was performed on CT26 tumor bearing mice in both control and dextran sodium sulfate (DSS) induced colitis settings. Spontaneous adenomas in genetically engineered mouse (GEM) models of colon cancer were additionally imaged. The EGFR imaging agent was generated with high purity (> 98%), with a labeling efficiency of 60 ± 5% and ≥99% radiochemical purity. The KD was 6.6 ± 0.7 nM and the Bmax for CT26 cells was 3.3 ± 0.1 × 106 receptors/cell. Target to background ratios (TBR) for CT26 tumors compared to colonic uptake demonstrated high values for both 18F-FDG (3.95 ± 0.13) and the developed 64Cu-DOTA-cetuximab-F(ab′)2 probe (4.42 ± 0.11) in control mice. The TBR for the EGFR targeted probe remained high (3.78 ± 0.06) in the setting of colitis, while for 18F FDG, this was markedly reduced (1.54 ± 0.08). Assessment of the EGFR targeted probe in the GEM models demonstrated a correlation between radiotracer uptake in spontaneous colonic lesions and the EGFR staining level ex vivo. A clinically translatable PET imaging probe was successfully developed to assess EGFR. The imaging agent can detect colonic tumors with a high TBR for detection of in situ lesions in the setting of colitis, and opens the possibility for a new approach for screening high-risk patients.
Keywords: Positron emission tomography (PET) imaging, molecular imaging, EGFR, ulcerative colitis, colorectal cancer, mouse models.
Introduction
Inflammatory bowel disease (IBD), which consists of Crohn's disease (CD) and ulcerative colitis (UC), is a chronic inflammatory condition that results from dysregulation of the mucosal immune system in the gastrointestinal tract1. The incidence of IBD is increasing, and 1.4 million people in the United States and 2.2 million people in Europe are affected by the disease2. Colorectal cancer (CRC) is one of the most serious complications of IBD involving the colon, and is responsible for 10-15% of IBD deaths. CRC is curable at the early stages and early detection of CRC or colonic adenomas resulting from chronic inflammation is a major focus of current research studies to improve patient survival3. Endoscopic guided biopsy is the standard for the diagnosis of CRC and periodic colonoscopy examinations reduces the mortality risk in IBD-associated CRC4. However, the issues surrounding endoscopic screening are exacerbated in ulcerative colitis (UC), in which dysplasia can develop in macroscopically normal-appearing mucosa5. Current colonoscopic surveillance in UC patients relies on random biopsies throughout the colon, which is a relatively insensitive and cumbersome strategy that is not widely utilized6. Because periodic screening is essential to reduce the incidence of IBD-associated CRC, the development of better molecular imaging technologies to detect CRC in the setting of colitis could provide a new approach for screening in this setting.
Positron emission tomography (PET) is of considerable importance to clinicians in the staging and treatment planning in patients with CRC7. 18F-Fluorodeoxyglucose (FDG) is a glucose analog that is the most widely employed PET radioligand in oncology, given the increased glycolysis rate often observed in tumors. However, inflammatory cells are also glycolytically active8, and 18F FDG has been used to monitor the degree of active inflammation in IBD8-10. Improved differentiation between neoplastic and nonneoplastic lesions is important in target selection for molecular imaging11. Detection of the increased glycolytic activity of CRC in the setting of increased glycolytic activity seen in IBD may result in a poor target to background ratio (TBR) for 18F-FDG.
We hypothesized that highly expressed epitopes on CRC tumor cells may provide an alternative target for imaging in this setting. We noted that epidermal growth factor receptor (EGFR) overexpression is present in approximately 80% of CRC cases, correlated with poor prognosis, decreased survival, and early recurrence12. While EGFR overexpression by itself does not directly result in utility as a therapeutic target, based in part on downstream K-RAS and additional signaling requirements13, the high rate of overexpression may be exploited as a target for lesion detection14. Inflammatory cell lineages do not overexpress EGFR, and thus in the setting of colitis, imaging based on EGFR expression may result in high TBR for detection of in situ cancer15. We developed a novel EGFR targeted PET imaging agent and tested the probe to assess radioligand uptake in colon cancer allografts, spontaneous colonic adenomas in genetically engineered mouse models, and in chemically induced colitis. We compared the TBR for allografts and colitis for the EGFR targeted probe relative to 18F-FDG.
Materials and Methods
Preparation of F(ab′)2 fragments
Cetuximab F(ab′)2 fragments were prepared by specific enzymatic digestion using a FragIT™ MicroSpin column (Genovis, Lund, Sweden) and the crude digest was purified by an immobilized NAb™ Protein A spin column (ThermoScientific Sci, Rockford, IL, USA) to remove the Fc fragment. The purity of cetuximab-F(ab′)2 was assessed with sodium dodecyl sulfate polyacrylamide gel electrophoresis (SDS-PAGE) on a 4-15% Mimi-PROTEAN® TGX mini-gel (Bio-Rad, Mississauga, ON, Canada) and with fast protein liquid chromatography (FPLC). F(ab′)2 was electrophoresed under non-reducing conditions with SDS-PAGE and the gel was stained with Bio-Safe™ Coomassie G-250 stain (Bio-Rad, Mississauga, ON, Canada). FPLC was performed on a HIPREP™ 26/60 Sephacryl™ S-200 HR column (GE Healthcare Bio-Sciences AB, Björkgatan, Uppsala, Sweden) and eluted with 100 mM NaH2PO4 buffer (pH 7.0) at a flow rate of 1.2 mL/min at 280 nm. Trace metals were removed from all buffers using Chelex®-100 cation-exchange resin (Sigma-Aldrich, Saint Louis, MO, USA). Cetuximab-F(ab′)2 fragments were concentrated and buffer-exchanged into 0.1 M HEPES buffer, pH 8.9 on an Amicon Ultracel 30 K device (MWCO= 30 kDa; EMD Millipore Corporation, Billerica, MA, USA)16. Cetuximab-F(ab′)2 was conjugated with the bifunctional 2-(4-isothiocyanatobenzyl)-1,4,7,10-tetraazacyclodo-decane-1,4,7,10-tetraacetic acid (p-SCN-Bn-DOTA, Macrocyclics, Inc., Dallas, TX, USA) chelate in anhydrous DMSO by a modification of established methods using 10 fold molar excess of chelate to cetuximab F(ab′)217, 18. Conjugation was allowed to proceed overnight at 2-8 °C. DOTA-cetuximab- F(ab′)2 was purified from excess DOTA by the Amicon Ultracel 30 K device with 0.25 M ammonium acetate buffer (pH 6.0) and centrifuging at 3500 rpm for 10 min. This purification step was repeated six times. Finally, purified DOTA-cetuximab-F(ab′)2 was recovered and the concentration determined spectrophotometrically [E280 nm = 1.45 (mg/mL)-1 cm-1]19. The final concentration was adjusted with 0.25 M ammonium acetate buffer (pH 6.0) for aliquoting.
The DOTA substitution level of the F(ab′)2 fragments (chelators/molecule) was measured by labeling a 10 μL aliquot of the unpurified conjugate with 67Ga and then determining the proportion of 67Ga-DOTA-cetuximab-F(ab′)2 vs. free 67Ga-DOTA by ITLC-SG and multiplying this fraction by the molar ratio used in the reaction19.
Radiolabeling procedures
Radiolabeling was done with 67Ga (MDS-Nordion, Kanata, Canada) or 64Cu (University of Wisconsin, Madison, WI) as described previously20, 21. We used 67Ga for cell binding assays due to its relatively longer half-life (3.26 d) in comparison with 64Cu (0.529 d) and lower energy, facilitating the cell study workflow. Briefly the 67Ga radioisotope (1-5 mCi) was added to the conjugate (50-100 μg) dissolved in 10 mM sodium acetate buffer (pH 4.5) and then incubated at 40ºC for 90 min. 64Cu radiolabeling was performed by incubating 50-100 μg of DOTA-cetuximab-F(ab′)2 in 0.25 M ammonium acetate buffer (pH 6.0) with 64CuCl2 for 90 min at 40°C with constant shaking. The 67Ga/64Cu-radiolabeled compounds were purified from free 67Ga /64Cu and other low molecular weight impurities on an Amicon Ultracel 30 K device. The purity of the labeled compounds were checked by size exclusion chromatography using a PD-10 Desalting Column (GE Healthcare Bio-Sciences AB, Björkgatan, Uppsala, Sweden) eluting with phosphate-buffered saline (PBS) as the mobile phase. The two different isotopes were used for in vivo and in vitro studies, in order to more closely match the isotope half-lives with the differences in length of the respective studies.
Cell culture
CT26 murine colorectal carcinoma and HCT-116 human colorectal carcinoma were obtained from the American Type Culture Collection (ATCC). They were cultured in RPMI and McCoy's 5a Medium (ATCC) and supplemented with 10% (v/v) fetal bovine serum (FBS), 100 U/mL penicillin, and 100 μg/mL streptomycin respectively. The cells were maintained in a humidified atmosphere of 5% CO2 at 37 ºC.
Competitive binding studies
The EGFR binding affinity of 67Ga-DOTA-cetuximab-F(ab′)2 was determined by direct (saturation) radioligand binding assays in triplicate using a fixed concentration of cetuximab and increasing concentration of 67Ga-DOTA-cetuximab-F(ab′)2 on the CT26 cell line with slight modification of previous studies22. Briefly, increasing concentrations (0 to 100 nmol/L) of 67Ga-DOTA-cetuximab-F(ab′)2 was incubated with 1 X 105 cells in 24-well plates at 4°C for 3 hr. Unbound radioactivity was removed and the dishes were rinsed three times with ice cold PBS and cells detached with 0.05% trypsin. The number of cells in each well was counted using an automated cell counter (Countess®, Invtrogen, NY, USA) and the total cell-bound radioactivity (TB) was measured in a gamma counter (Wizard 2480, Perkin Elmer, MA, USA). The assay was repeated in the presence of 16 μmol/L of unlabeled cetuximab to measure non-specific binding (NSB) at 4ºC for 2h. Specific binding (SB) was calculated by subtracting NSB from TB and was plotted vs. the concentration of 67Ga-DOTA-cetuximab-F(ab′)2 added. The resulting curve was fitted by non-linear regression to a one-site receptor-binding model by Prism software (GraphPad, San Diego, CA, USA). The dissociation constant (KD) and maximum number of receptors per cell (Bmax) was calculated.
Western Blot Analysis
In order to ensure EGFR expression in CT26 and HCT-116 cells, Western blot analysis was carried out as previously described23. EGFR expression level of CT26 was compared with the high EGFR expressing HCT116 human colon cancer cell line. Briefly, EGFR and beta-actin were detected with EGFR receptor XP rabbit mAb (Cell Signaling, Danvers, MA, USA) (1:1000 dilution) and beta-actin rabbit mAb (Cell Signaling, Danvers, MA, USA) (1:1000 dilution). Then the proteins were incubated with goat anti-rabbit IgG-HRP (Santa Cruz Biotechnology, Inc., Santa Cruz, CA, USA) and detected using the BM chemiluminescence Western blotting kit (Roche Diagnostics, Indianapolis, IN, USA) and bands were visualized with a Kodak in vivo FX PRO system (Carestream Health, New Haven, CT, USA).
Animal models
All animal experiments were approved by our Institutional Animal Care Committee. Mice were maintained with free access to standard chow and water. Female BALB/c mice (6 weeks old, with a body weight of 18-20 g) were purchased from Charles River Laboratories International Inc. Dextran Sulfate Sodium (DSS)-treated mice were prepared by the administration of 3.0% DSS (mol wt 40,000-50,000, MP Affymetrix, Inc., Cleveland, Ohio, USA.) in drinking water for seven days, followed by a regimen of three days of normal drinking water, as described previously24. Control mice received water ad libitum. Fresh DSS solutions were prepared daily and mice were recorded daily for the body weight loss, which was calculated relative to day 0. Subcutaneous (s.c) CT26 tumors were established in a subset of BALB/C mice by s.c injection of 100 μL (106 cells) of CT26 cell suspension in Matrigel (BD Biosciences, Franklin Lakes, NJ, USA) in the right upper flank.
To further assess the imaging method, mice with conditional knockout (CKO) mutant alleles were generated as previously described25, 26, 27, 28 and ApcCKOp53flox/flo and ApcLoxP/ LoxPMsh2null/LoxP mutant mouse models were used to evaluate the imaging potential of 64Cu-DOTA-cetuximab-F(ab′)2 in CRC.
PET/CT imaging protocol
Before imaging with 18F-FDG, the mice were kept fasted for 4 hr and allowed free access to water. For PET/CT imaging, approximately 400 μCi of 18F-FDG or 100 μCi of 64Cu-DOTA-cetuximab-F(ab′)2 in a final volume of 200 μl was injected to each mouse via the tail vein under 2% isoflurane gas anesthesia.
PET data were acquired using a whole-body emission protocol on an Argus small-animal PET/CT scanner (Sedecal, Madrid, Spain) for 15 min in 2 bed positions 1 hr after 18F-FDG and 24 hr after 64Cu-DOTA-cetuximab-F(ab′)2 injection under gas anesthesia with 1.5% isoflurane. Images were reconstructed with a 2D ordered-subset expectation maximization (2D-OSEM) algorithm (2 iterations, 16 subsets, with scatter and randoms corrections). CT data were acquired in standard resolution. The scan parameters were set as follow: tube voltage 40 kVp, tube current 140 µA, number of projections 360, number of shots 8, axial field-of-view 80 mm. Scans were recorded without respiratory gating. Total scan duration was approximately 14 min. Image data were reconstructed using FeldKemp algorithm. Three-dimensional regions of interest (ROI) were manually drawn around tumors based on co-registered CT scans acquired immediately after PET imaging. Mean standardized uptake values (SUVs) were calculated within the ROI.
Antibody blocking studies
Blocking studies were carried out to evaluate EGFR specificity of 64Cu-DOTA-cetuximab-F(ab′)2 in vivo. Mice bearing CT26 allografts (n=4) were each intravenously injected with 1.5 mg of cetuximab 24 hr before 64Cu-DOTA-cetuximab-F(ab′)2 administration. The control group mice with CT26 allografts (n=4) were injected with intravenous PBS 24 hr before 64Cu-DOTA-cetuximab-F(ab′)2 injection. 64Cu-DOTA-cetuximab-F(ab′)2 was intravenously injected into each mouse under isoflurane anesthesia and static PET/CT scans were acquired at 24 hr post injection. Mean standardized uptake values (SUVs) of the allografts were calculated and compared between groups.
PET/CT imaging with 18F-FDG and 64Cu-DOTA-cetuximab-F(ab′)2
PET was performed to quantitate the effect of intestinal inflammation upon bowel 18F-FDG uptake, as measured in BALB/c mice induced with DSS. 18F-FDG was purchased from IBA. A baseline 18F-FDG PET/CT was performed on day 0 to ensure that the subject mice have no baseline bowel pathology that enhanced glucose uptake.
The DSS-treated (n=4) and control mice (n=4) with CT26 s.c allografts were imaged with 18F-FDG and 64Cu-DOTA-cetuximab-F(ab′)2 PET/CT and tumor to bowel ratios were compared between the DSS-treated mice and control group for both radiotracers (18F-FDG and 64Cu-DOTA-cetuximab-F(ab′)2 ).
Conditional knockout mice with ApcCKOp53flox/flox and ApcLoxP/ LoxPMsh2null/LoxP mutation underwent whole body PET/CT imaging 24 hr after intravenous 64Cu-DOTA-cetuximab-F(ab′)2 injection. The colons of the mice were extracted immediately after whole body PET/CT and were placed in the PET/CT scanner for ex vivo imaging. The static ex vivo PET/CT images from these colons were overlaid on the gross white light photographs of the colons in the same position and orientation.
Histological analysis
Mice were euthanized and the colons were removed, and cleaned in physiological saline solution to remove fecal residue. They were fixed in neutrally buffered 10% formalin at room temperature for 48 hr before they were embedded in paraffin and sectioned. All tissues were stained with hematoxylin and eosin (H&E) for histological evaluation. Light microscopy was performed with an Olympus IX51 microscope.
Immunohistochemical (IHC) analysis was performed on CT26 tumor allografts, and colon tissue samples as described previously1, 7. Briefly, unstained 5 μm sections were cut, deparaffinized and rehydrated by standard techniques before antigen retrieval in EDTA buffer. The samples were then incubated in a 1:50 dilution of anti-EGFR rabbit polyclonal IgG (Santa Cruz Biotechnology, Inc., Santa Cruz, CA, USA) overnight at 4 ºC. The sections were washed in TBST and incubated with biotinylated goat anti-rabbit IgG (H+L) (Abcam, Cambridge, MA, USA) for 1 hr. The staining was developed using the DAKO Liquid DAB + substrate chromogen system (Dako, Carpinteria, CA, USA) for 1 min. Slides were washed in water and counterstained with hematoxylin and dehydrated before mounting.
Statistics
Statistical analysis was performed using Prism software (Graphpad, San Diego, USA). Differences in uptake of the tracers were tested for significance using the t-test. P-values of 0.05 were considered significant. Data are represented as mean ± standard error of the mean (SEM).
Results
Radiotracer preparation and characterization
F(ab′)2 fragment of cetuximab was produced through enzymatic digestion as shown in Figure 1A. F(ab′)2 was generated with high purity (> 98%) and 1.2 mg F(ab′)2 was recovered from 2 mg of antibody (~60% yield). The size-exclusion FPLC and SDS-PAGE results demonstrated that pure F(ab′)2 fragment of cetuximab was obtained after the digestion of intact IgG with enzymatic digestion and followed by protein A purification (Figure 1B&C). Whole antibody appears at 180 min, while F(ab′)2 appears at 202 min and Fc appears at 235 min (Figure 1B). Reaction of cetuximab F(ab′)2 with a 10-fold excess of p-SCN-Bn-DOTA resulted in substitution of approximately 1 DOTA chelate per F(ab′)2. The labeling efficiency for 64Cu-DOTA-cetuximab-F(ab′)2 was 60 ± 5% and with ≥99% radiochemical purity (Figure 1D). The specific activity of 64Cu-DOTA-cetuximab-F(ab′)2 was 19.5 ± 6.8 mCi/mg cetuximab.
A schematic overview of the EGFR targeted PET probe synthesis and characterization. (A) Enzymatic fragmentation of whole antibody and conjugation of F(ab')2 fragment with bifunctional chelator. (B) FPLC chromatograms of whole IgG before digestion, after digestion, and after protein A purification. (C) SDS-PAGE analysis of enzymatic digestion of cetuximab IgG. (i) Whole antibody before digestion; (ii) F(ab')2 and Fc bands after digestion of whole antibody; (iii) F(ab')2 band after protein A purification. (D) Radiolabeling and purification of F(ab')2-DOTA conjugate with 67Ga. (E) Direct (saturation) radioligand binding to CT26 murine colorectal cancer cells of 64Cu-DOTA-cetuximab-F(ab')2, in the absence (total binding; TB) or presence (non-specific binding; NSB) of excess (x 20 times) unlabeled cetuximab IgG. Specific binding (SB) was calculated by subtraction of NSB from TB. Curves were fit to a 1-site receptor-binding model. ◆= TB; ■= NSB; ▴= SB. (F) Western blot of EGFR expression in CT26 and HCT-116 colon cancer cell lines with beta-actin as control, demonstrate EGFR overexpression.
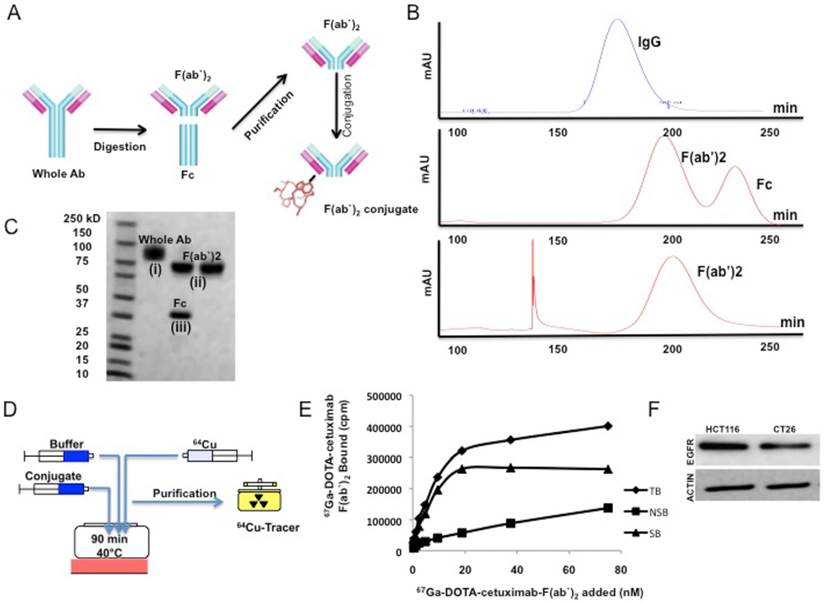
We observed that CT26 murine colon cancer cell line has high EGFR expression, comparable to that of high EGFR expressing HCT-116 human colorectal cancel line as shown in Western blot analysis (Figure 1F). Direct (saturation) radioligand binding assays showed that64Cu-DOTA-cetuximab-F(ab′)2 bound specifically to EGFR on CT26 cells (Figure 1E). The KD value for 64Cu-DOTA-cetuximab-F(ab′)2 was 6.6 ± 0.7 nM and the Bmax value on CT26 cells was 3.3 ± 0.1 × 106 receptors/cell. A representative competitive binding curve of 64Cu-DOTA-cetuximab-F(ab′)2 is shown in Figure 1E.
The 64Cu-DOTA-cetuximab-F(ab′)2 is specific for EGFR in vivo
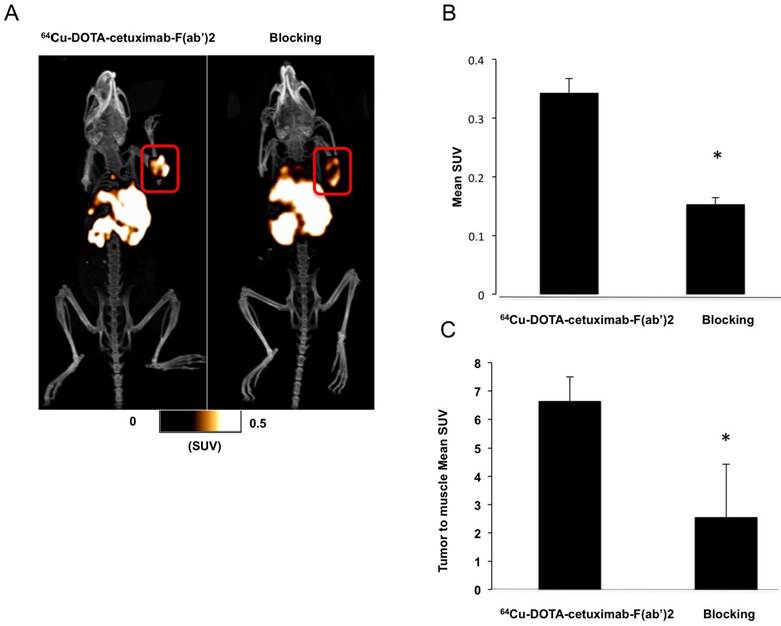
The specificity of 64Cu-DOTA-cetuximab-F(ab′)2 for EGFR was confirmed by in vivo blocking studies (Figure 2). Administering a blocking dose of cetuximab the tumor uptake was significantly reduced (SUV of 0.31 ± 0.04 (non-blocking) vs. 0.15 ± 0.02 (blocking), n=4; P<0.05) and (tumor to muscle SUV of 6.64 ± 0.85 (non-blocking) vs. 2.56 ± 1.87 (blocking), n=4; P<0.05) which demonstrated that 64Cu-DOTA-cetuximab-F(ab′)2 maintained EGFR specificity in vivo.
PET imaging of EGFR expression in BALB/c mice at 24 hr post injection of 64Cu-DOTA-cetuximab-F(ab′)2 or 64Cu-DOTA-cetuximab-F(ab')2 after treatment with a 1.5 mg blocking dose of cetuximab. A) Example images without and with blocking. Red circles highlight site of implanted CT26 tumor allograft B) Comparison of MeanSUV values of 64Cu-DOTA-cetuximab-F(ab′)2 without and with blocking. Each bar represents SUVmean ± SEM; n=4 for each group, and the symbol * denotes P<0.05. C) Comparison of tumor to muscle ratios of 64Cu-DOTA-cetuximab-F(ab′)2 without and with blocking. Each bar represents SUVmean ± SEM; n=4 for each group, and the symbol * denotes P<0.05.
The DSS induced colitis model
Body weight loss was used to monitor colitis. The body weight loss gave a peak on day 8 (Figure 3A). The body weight was significantly decreased (23.35 ± 0.11 g (day 0) vs. 20.45 ± 0.64 g (DSS-treated, day 8) and 23.35 ± 0.11 g (day 0) vs. 20.35 ± 0.21 (DSS-treated, day 10), n=4, P<0.05) after DSS treatment. PET imaging was performed on control and DSS-treated mice to assess the effects of colitis on 18F-FDG colonic uptake after DSS treatment. The arrows on the images indicate the high characteristic accumulation of 18F-FDG in the inflamed areas of DSS-treated mice (Figure 3B). 18F-FDG PET/CT scans showed significant increase in uptake (0.22 ± 0.02 %ID/g (control) vs. 0.43 ± 0.09 %ID/g (DSS-treated, day 9), n=4, P<0.05) in the colons of the DSS-treated groups.
Assessment of symptoms and histological findings of DSS-treated and control mice. BABL/c mice were subjected to 3% DSS for seven days and followed with normal drinking water for three days. (A) Body weight changes following DSS induction of colitis, reported as mean ± SEM (n=4 mice/group) and the symbol * denotes P<0.05. (B) microPET-CT scans were obtained before and after DSS treatment. Before DSS treatment, PET showed only low level of physiologic 18F-FDG uptake in the colon of healthy controls. In contrast, on day nine, clearly elevated 18F-FDG colonic uptake is noted (red arrow). (C) Histological appearance of the normal colonic mucosa of healthy controls with intact crypts and architecture (control) and DSS-induced colitis showing inflammatory infiltration (arrow head), mucin loss (arrow) and crypt architectural disarray (dashed arrow). Magnification x20 and scale bar represents 100 μm.
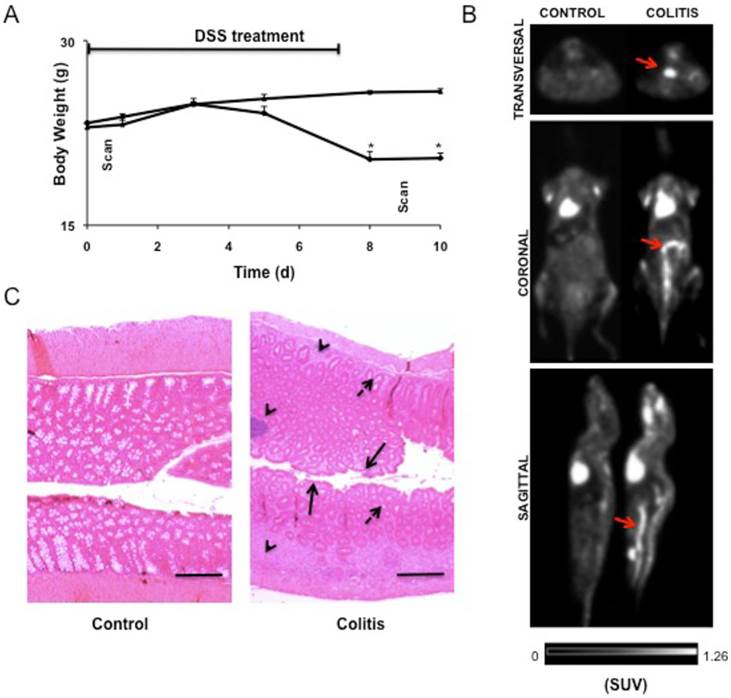
Histological examination of the normal colon showed normal mucosal architecture. Mucin loss, loss of crypt architecture and intraepithelial inflammation was observed in the colon of mice that received DSS treatment for seven days (Figure 3C).
PET/CT imaging
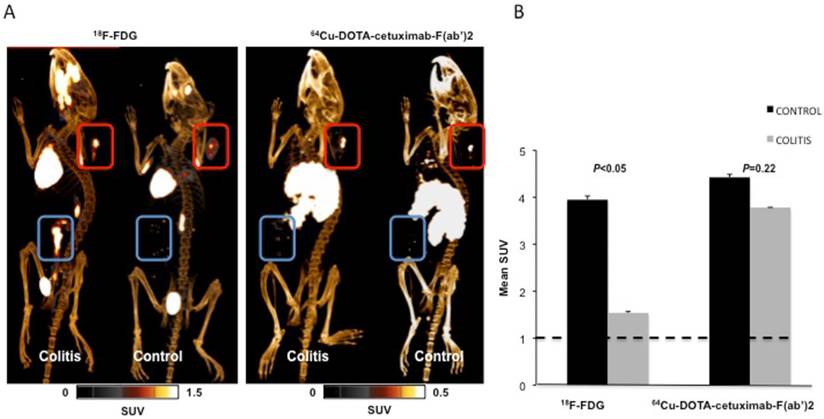
In a subset of control and DSS-treated BALB/C mice implanted with CT26 allografts imaging was performed sequentially with both 18F-FDG and 64Cu-DOTA-cetuximab- F(ab′)2 to compare the tumor to bowel radiotracer uptake ratios (Figure 4A). The tumor to bowel ratio was significantly decreased (3.95 ± 0.13 (control) vs. 1.54 ± 0.08 (DSS-treated), n=4, P<0.05) in DSS-treated mice imaged with 18F-FDG. However there was no significant difference (4.42 ± 0.11 (control) vs. 3.78 ± 0.06 (DSS-treated), n=4, P=0.22) in the tumor to bowel ratio between the control and the DSS-treated mice imaged with 64Cu-DOTA-cetuximab-F(ab′)2. 64Cu-DOTA-cetuximab-F(ab′)2 also showed significantly higher (3.78 ± 0.06 (64Cu-DOTA-cetuximab-F(ab′)2) vs. 1.54 ± 0.08 (18F-FDG), n=4; P<0.05) tumor to bowel ratio in comparison with 18F-FDG in DSS-induced mice (Figure 4B).
Comparison of PET imaging with 18F-FDG and 64Cu-DOTA-cetuximab-F(ab′)2 in CT26 tumor-bearing mice with and without DSS-induced colitis. (A) PET-CT images were performed 1 hr after 18F-FDG and 24 hr after 64Cu-DOTA-cetuximab-F(ab')2 administration. Representative images from a mouse are shown, with n=4 mice imaged in each group. Red squares indicate the location of tumors and blue squares indicate location of DSS-induced colitis. (B) Comparison of tumor to colon ratios at 24 hr post-injection. Each bar represents SUVmean ± SEM; n=4 for each group. The symbol * denote P<0.05 and the difference is not significant (P=0.22) for 64Cu-DOTA-cetuximab-F(ab′)2. The dash line verifies TBR=1 (no contrast).
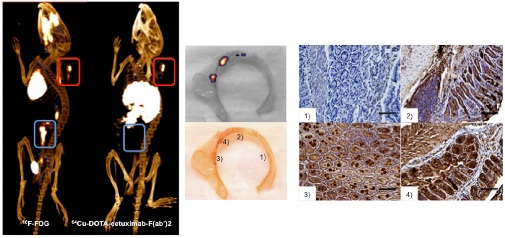
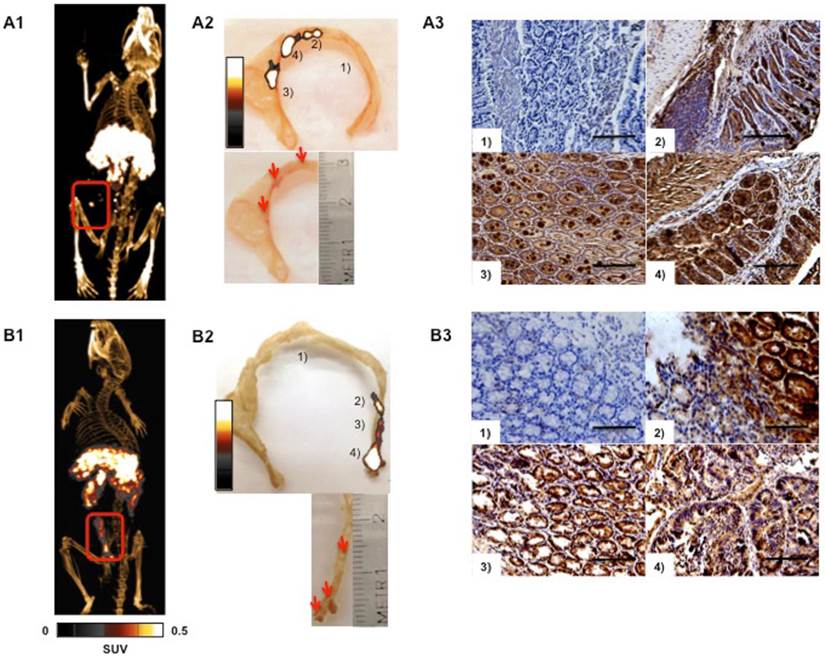
64Cu-DOTA-cetuximab-F(ab′)2 whole body PET/CT images of mice with ApcCKOP53flox/flox and ApcLoxP/ LoxPMsh2null/LoxP mutations revealed focal areas of high uptake in colonic adenomas. After the PET/CT imaging, the colons were excised and imaged ex vivo with PET/CT. An anatomic correlation between the location of visible adenoma foci and areas of high uptake in ex vivo 64Cu-DOTA-cetuximab-F(ab′)2 PET/CT images was noted. (Figure 5A&B).
Correlation between EGFR targeted PET imaging and EGFR immunohistochemistry. (A1) PET imaging of ApcCKOP53flox/flox mouse with 64Cu-DOTA-cetuximab-F(ab′)2 at 24 hr. (A2) The digital photograph of colon and the colon fused with the ex-vivo PET image. (A3) Corresponding EGFR expression patterns of different colon sections numbered in A2 are confirmed with immunohistochemistry (magnification x20). (B1) Representative images of decay corrected PET image of ApcLoxP/ LoxPMsh2null/LoxP mutant mice after the injection of 64Cu-DOTA-cetuximab-F(ab′)2 at 24 hr. (B2) The digital photograph of colon and the colon fused with the ex-vivo PET image. (B3) EGFR expression patterns of different colon sections numbered in B2 are confirmed with immunohistochemistry (magnification x20). Scale bar represents 50 μm.
Histopathologic analysis
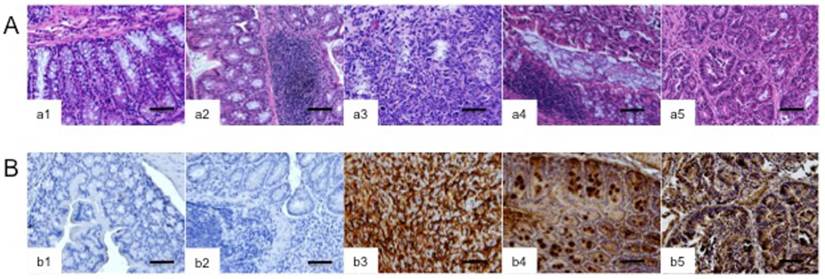
H&E and IHC stained tissue sections of mice are shown in Figure 6. Normal colonic mucosa with crypt architecture, along with modulation seen with DSS-treatment, and characteristic features in the adenomas are noted (Figure 6A). Membranous brown staining of cells above the background level was defined as EGFR positive. IHC staining for EGFR revealed very weak staining in control and DSS-treated colonic tissue, while strong EGFR staining was observed with CT26 allograft and colon tumors from ApcCKOp53flox/flox and ApcLoxP/ LoxPMsh2null/LoxP mutant mice (Figure 6B). Interestingly, the level of IHC staining for EGFR for the adenomatous lesions visually corresponds with the level of vivo 64Cu-DOTA-cetuximab-F(ab′)2 uptake in the ex vivo samples (Figure 5).
H&E and IHC analysis were examined to compare the histological changes in colons from healthy, DSS-treated, GEM models and allograft (CT26 tumor). IHC results demonstrate that there is no significant EGFR expression in healthy and DSS-treated colons, while there is strong staining in allograft and GEM model colonic lesions. (A) Representative H&E tissue sections from (a1) healthy colon, (a2) DSS-treated colon, (a3) CT26 allograft, (a4) ApcCKOP53flox/flox mutant mouse colon, (a5) ApcLoxP/LoxPMsh2null/LoxP mutant mouse colon. (B) IHC analysis of EGFR from tissues of (b1) healthy colon, (b2) DSS-treated colon, (b3) CT26 allograft, (b4) ApcCKOP53flox/flox mutant mouse colon, (b5) ApcLoxP/ LoxPMsh2null/LoxP mutant mouse colon. Scale bar represents 50 μm.
Discussion
Persistent inflammation in the colon seen in IBD is correlated with increased cell proliferation, dysplasia, and the subsequent development of CRC4, 29-31. The mortality of IBD associated CRC has remained high over the last 20 years, in part due to the approximately 50% of CRC that were not detected until an advanced stage32. Therefore there is a clear need to develop new screening strategies that are more sensitive and less cumbersome than current approaches for high-risk patients. While the noninvasive nature of PET scanning greatly improves tolerance, colonic inflammation that is a hallmark of IBD affecting the colon makes noninvasive screening for cancer using 18F-FDG PET somewhat less useful in the IBD setting, given the known uptake of the radiotracer in inflammatory as well as neoplastic cells. We hypothesized that EGFR would be an appropriate target for imaging, highlighting tumor even in the setting of colitis, given its high expression seen in the large majority of CRC, and the lack of overexpression noted in normal colonic mucosa and in the inflammatory cells associated with chronic colitis. We thus developed an EGFR targeting PET imaging agent based on the F(ab′)2 fragment of cetuximab conjugated to the chelator DOTA and labeled with the radiometal 64Cu. We chose the F(ab′)2 fragments as the basis for the imaging agent given the improved target to background ratio (TBR) relative to whole antibodies33, and improved pharmacokinetics for translation16, 34. The developed imaging agent is translatable for human studies given the high safety profile of the parent antibody, and the components have all been utilized in prior clinical translation. PET imaging agents have an advantage of an extremely low mass of injection given the high sensitivity of PET detection, and thus a broad range of agents have been translated to human evaluation35. Finally, as new algorithms are developed for image reconstruction and with the introduction of PET-MR clinical scanners, the radiation dose associated with PET imaging continues to decrease, making this potential approach more appealing36. While very low bowel uptake was seen in these preclinical studies in both normal and colitis settings, given the known hepatic clearance, early translational studies will help confirm that low signal from bowel remains in the clinical setting.
Monoclonal antibodies are widely used as therapeutics. However, their long circulation time typically in the range of days to weeks, and the potential for immune response, make their use as imaging agents less ideal37-39. Bivalent F(ab′)2 antibody fragments have a shorter blood clearance, higher tumor to background ratios at early time points, reduced non-specific distribution, and lower immunogenicity relative to whole antibodies, while retaining the advantage of increased affinity associated with bivalency16, 40. The developed imaging probe has a high affinity of 6.6 nM for EGFR. We chose a radioisotope, 64Cu (t1/2 = 12.7 h), that matched the pharmacokinetics of the F(ab′)2 antibody fragment39. We demonstrated that the EGFR targeting probe was able to image both allografts (CT26 tumors) as well as spontaneous colonic adenomas in two different GEM models (ApcCKOp53flox/flo and ApcLoxP/ LoxPMsh2null/LoxP)25-28 with high standard uptake values (SUV). In the previous studies, Western blots of EGFR expression on human and murine cell lines showed that cetuximab strongly binds to the murine cell line CT2641. GEM models are selected to provide a platform for studying CRC from certain mutations such Apc and p53. ApcCKOp53flox/flo and ApcLoxP/ LoxPMsh2null/LoxP GEM models were selected for this study because Apc and Msh2 processes are often deranged in large numbers of CRCs in the setting of IBD42, 43. The EGFR targeted probe uptake in spontaneous lesions in representative mouse models of colonic adenomas further points to the translational potential of this approach. Both 18F-FDG and 64Cu-DOTA-cetuximab- F(ab′)2 demonstrated high TBR for tumor uptake relative to normal colon. However, the EGFR targeting probe retained a high TBR in the setting of colitis, whereas the TBR markedly decreased for 18F-FDG to approximately 1.5 in the setting of bowel inflammation, largely due to the expected increase in 18F-FDG uptake in the inflamed bowel.
A large percentage of IBD-associated cancers have immunohistochemical positivity for EGFR and strong EGFR intensity has been associated with higher tumor staging44, 45, 46. Our results show a strong correlation between whole body PET-CT EGFR-targeted imaging, ex-vivo EGFR-based PET imaging of the colon, and histopathological findings of the degree of EGFR expression. The visualized weak EGFR staining of healthy colon is likely secondary to the limited EGFR expression in the basolateral surface of the colon23. We additionally confirmed the previously reported weak EGFR staining for DSS-induced colitis 47. High EGFR staining was clearly visualized in the CT26 allograft and colorectal adenomas in the GEMM. It has been previously noted that the mean specific EGFR intensity in neoplasia is approximately ten times higher than in normal mucosa12. Given the high correlation between lesion EGFR expression and uptake of the developed 64Cu-DOTA-F(ab′)2 PET imaging probe, the approach may be useful not only for detection, but also for anti-EGFR treatment monitoring.
Conclusions
A clinically translatable 64Cu-DOTA-cetuximab-F(ab′)2 PET imaging probe was successfully developed to assess EGFR noninvasively. The imaging agent can detect colonic tumors with a high target to background ratio in the setting of colitis. This approach offers improved imaging characteristics compared to standard 18F-FDG PET imaging for detection of in situ lesions in the setting of IBD, and opens the possibility for a new approach for screening high-risk patients for the development of CRC in the setting of colonic inflammation.
Acknowledgements
This study was supported by U01CA084301, P50CA127003, and U01CA143056. N. Selcan Turker supported by the Dubai Harvard Foundation for Medical Research (DHFMR, grant number: 223439).
Competing Interests
The authors have declared that no competing interest exists.
References
1. Lissner D, Siegmund B. Ulcerative colitis: current and future treatment strategies. Dig Dis. 2013;31:91-4
2. Burisch J, Munkholm P. Inflammatory bowel disease epidemiology. Curr Opin Gastroenterol. 2013;29:357-62
3. O'Connor OJ, McDermott S, Slattery J. et al. The Use of PET-CT in the Assessment of Patients with Colorectal Carcinoma. Int J Surg Oncol. 2011;2011:846512
4. Ahmadi A, Polyak S, Draganov PV. Colorectal cancer surveillance in inflammatory bowel disease: the search continues. World J Gastroenterol. 2009;15:61-6
5. Kiesslich R, Fritsch J, Holtmann M. et al. Methylene blue-aided chromoendoscopy for the detection of intraepithelial neoplasia and colon cancer in ulcerative colitis. Gastroenterology. 2003;124:880-8
6. Bernstein CN, Weinstein WM, Levine DS. et al. Physicians' perceptions of dysplasia and approaches to surveillance colonoscopy in ulcerative colitis. Am J Gastroenterol. 1995;90:2106-14
7. Higashikawa K, Akada N, Yagi K. et al. Exploration of target molecules for molecular imaging of inflammatory bowel disease. Biochem Biophys Res Commun. 2011;410:416-21
8. Bettenworth D, Reuter S, Hermann S. et al. Translational 18F-FDG PET/CT imaging to monitor lesion activity in intestinal inflammation. J Nucl Med. 2013;54:748-55
9. Berthold LD, Steiner D, Scholz D. et al. Imaging of chronic inflammatory bowel disease with 18F-FDG PET in children and adolescents. Klin Padiatr. 2013;225:212-7
10. Perlman SB, Hall BS, Reichelderfer M. PET/CT imaging of inflammatory bowel disease. Semin Nucl Med. 2013;43:420-6
11. Mahmood U. Optical molecular imaging approaches in colorectal cancer. Gastroenterology. 2010;138:419-22
12. Goetz M, Ziebart A, Foersch S. et al. In vivo molecular imaging of colorectal cancer with confocal endomicroscopy by targeting epidermal growth factor receptor. Gastroenterology. 2010;138:435-46
13. Heinemann V, Stintzing S, Kirchner T. et al. Clinical relevance of EGFR- and KRAS-status in colorectal cancer patients treated with monoclonal antibodies directed against the EGFR. Cancer Treat Rev. 2009;35:262-71
14. Hoetker MS, Kiesslich R, Diken M. et al. Molecular in vivo imaging of gastric cancer in a human-murine xenograft model: targeting epidermal growth factor receptor. Gastrointest Endosc. 2012;76:612-20
15. Dube PE, Yan F, Punit S. et al. Epidermal growth factor receptor inhibits colitis-associated cancer in mice. J Clin Invest. 2012;122:2780-92
16. Wong KJ, Baidoo KE, Nayak TK. et al. In Vitro and In Vivo Pre-Clinical Analysis of a F(ab')(2) Fragment of Panitumumab for Molecular Imaging and Therapy of HER1 Positive Cancers. EJNMMI Res. 2011 1
17. Cooper MS, Ma MT, Sunassee K. et al. Comparison of (64)Cu-Complexing Bifunctional Chelators for Radioimmunoconjugation: Labeling Efficiency, Specific Activity, and in Vitro/in Vivo Stability. Bioconjug Chem. 2012
18. Ferreira CL, Yapp DT, Crisp S. et al. Comparison of bifunctional chelates for (64)Cu antibody imaging. Eur J Nucl Med Mol Imaging. 2010;37:2117-26
19. Chan C, Scollard DA, McLarty K. et al. A comparison of 111In- or 64Cu-DOTA-trastuzumab Fab fragments for imaging subcutaneous HER2-positive tumor xenografts in athymic mice using microSPECT/CT or microPET/CT. EJNMMI Res. 2011;1:15
20. Ferreira CL, Lamsa E, Woods M. et al. Evaluation of Bifunctional Chelates for the Development of Gallium-Based Radiopharmaceuticals. Bioconjug Chem. 2010
21. Ferreira CL, Yapp DT, Mandel D. et al. (68)Ga small peptide imaging: comparison of NOTA and PCTA. Bioconjug Chem. 2012;23:2239-46
22. Miao Z, Ren G, Liu H. et al. Small-animal PET imaging of human epidermal growth factor receptor positive tumor with a 64Cu labeled affibody protein. Bioconjug Chem. 2010;21:947-54
23. Playford RJ, Hanby AM, Gschmeissner S. et al. The epidermal growth factor receptor (EGF-R) is present on the basolateral, but not the apical, surface of enterocytes in the human gastrointestinal tract. Gut. 1996;39:262-6
24. Whittem CG, Williams AD, Williams CS. Murine Colitis modeling using Dextran Sulfate Sodium (DSS). J Vis Exp. 2010
25. Martin ES, Belmont PJ, Sinnamon MJ. et al. Development of a colon cancer GEMM-derived orthotopic transplant model for drug discovery and validation. Clin Cancer Res. 2013;19:2929-40
26. Hung KE, Maricevich MA, Richard LG. et al. Development of a mouse model for sporadic and metastatic colon tumors and its use in assessing drug treatment. Proc Natl Acad Sci U S A. 2010;107:1565-70
27. Kucherlapati MH, Lee K, Nguyen AA. et al. An Msh2 conditional knockout mouse for studying intestinal cancer and testing anticancer agents. Gastroenterology. 2010;138:993-1002 e1
28. Kuraguchi M, Wang XP, Bronson RT. et al. Adenomatous polyposis coli (APC) is required for normal development of skin and thymus. PLoS Genet. 2006;2:e146
29. Fujii S, Fujimori T, Kawamata H. et al. Development of colonic neoplasia in p53 deficient mice with experimental colitis induced by dextran sulphate sodium. Gut. 2004;53:710-6
30. Eaden JA, Abrams KR, Mayberry JF. The risk of colorectal cancer in ulcerative colitis: a meta-analysis. Gut. 2001;48:526-35
31. Assadsangabi A, Lobo AJ. Diagnosing and managing inflammatory bowel disease. Practitioner. 2013;257:13-8 2
32. Liu S, Li D, Park R. et al. PET imaging of colorectal and breast cancer by targeting EphB4 receptor with 64Cu-labeled hAb47 and hAb131 antibodies. J Nucl Med. 2013;54:1094-100
33. Heskamp S, van Laarhoven HW, Molkenboer-Kuenen JD. et al. Optimization of IGF-1R SPECT/CT imaging using 111In-labeled F(ab')2 and Fab fragments of the monoclonal antibody R1507. Mol Pharm. 2012;9:2314-21
34. Tang Y, Wang J, Scollard DA. et al. Imaging of HER2/neu-positive BT-474 human breast cancer xenografts in athymic mice using (111)In-trastuzumab (Herceptin) Fab fragments. Nucl Med Biol. 2005;32:51-8
35. Mahmood U. MICoE Task Force Looks to the Future. J Nucl Med. 2009;50:15N
36. Cho IH, Han EO, Kim ST. Very different external radiation doses in patients undergoing PET/CT or PET/MRI scans and factors affecting them. Hell J Nucl Med. 2014;17:13-8
37. Zhang Y, Hong H, Orbay H. et al. PET imaging of CD105/endoglin expression with a (6)(1)/(6)(4)Cu-labeled Fab antibody fragment. Eur J Nucl Med Mol Imaging. 2013;40:759-67
38. Vlasak J, Ionescu R. Fragmentation of monoclonal antibodies. MAbs. 2011;3:253-63
39. Sihver W, Pietzsch J, Krause M. et al. Radiolabeled Cetuximab Conjugates for EGFR Targeted Cancer Diagnostics and Therapy. Pharmaceuticals (Basel). 2014;7:311-38
40. Tang Y, Scollard D, Chen P. et al. Imaging of HER2/neu expression in BT-474 human breast cancer xenografts in athymic mice using [(99m)Tc]-HYNIC-trastuzumab (Herceptin) Fab fragments. Nucl Med Commun. 2005;26:427-32
41. Cai W, Chen K, He L. et al. Quantitative PET of EGFR expression in xenograft-bearing mice using 64Cu-labeled cetuximab, a chimeric anti-EGFR monoclonal antibody. Eur J Nucl Med Mol Imaging. 2007;34:850-8
42. Kulendran M, Stebbing JF, Marks CG. et al. Predictive and prognostic factors in colorectal cancer: a personalized approach. Cancers (Basel). 2011;3:1622-38
43. Machin P, Catasus L, Pons C. et al. Microsatellite instability and immunostaining for MSH-2 and MLH-1 in cutaneous and internal tumors from patients with the Muir-Torre syndrome. J Cutan Pathol. 2002;29:415-20
44. Svrcek M, Cosnes J, Tiret E. et al. Expression of epidermal growth factor receptor (EGFR) is frequent in inflammatory bowel disease (IBD)-associated intestinal cancer. Virchows Arch. 2007;450:243-4
45. Rego RL, Foster NR, Smyrk TC. et al. Prognostic effect of activated EGFR expression in human colon carcinomas: comparison with EGFR status. Br J Cancer. 2010;102:165-72
46. Spano JP, Lagorce C, Atlan D. et al. Impact of EGFR expression on colorectal cancer patient prognosis and survival. Ann Oncol. 2005;16:102-8
47. Alexander RJ, Panja A, Kaplan-Liss E. et al. Expression of growth factor receptor-encoded mRNA by colonic epithelial cells is altered in inflammatory bowel disease. Dig Dis Sci. 1995;40:485-94
Author contact
Corresponding author: Umar Mahmood, MD. PhD. Athinoula A. Martinos Center for Biomedical Imaging, Department of Radiology, Massachusetts General Hospital, Boston, MA. Tel: 617-726-6477 Email: umahmoodharvard.edu.
 Global reach, higher impact
Global reach, higher impact