13.3
Impact Factor
Theranostics 2018; 8(5):1399-1410. doi:10.7150/thno.21072 This issue Cite
Research Paper
Mesenchymal stem cells-derived exosomes are more immunosuppressive than microparticles in inflammatory arthritis
1. Inserm, U1183, Saint-Eloi Hospital, Montpellier, France;
2. Montpellier University, UFR de Médecine, Montpellier, France;
3. Laboratorio de Inmunología Celular y Molecular, Centro de Investigación Biomédica, Facultad de Medicina, Universidad de Los Andes, Santiago, Chile,
4. Inserm, UMRs-970, Centre de Recherche Cardiovasculaire de Paris, PRES Sorbonne-Paris-Cité, Université Paris-Descartes, France;
5. Clinical immunology and osteoarticular diseases Therapeutic Unit, Hôpital Lapeyronie, Montpellier, France
*: equally contributing authors
Abstract
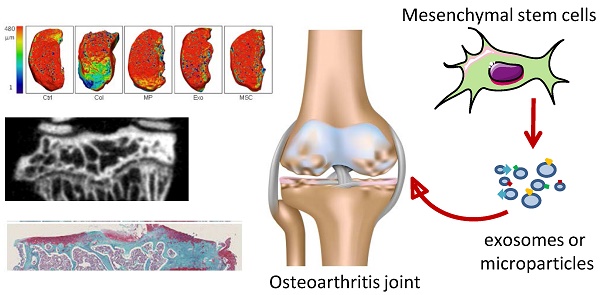
Objectives: Mesenchymal stem cells (MSCs) release extracellular vesicles (EVs) that display a therapeutic effect in inflammatory disease models. Although MSCs can prevent arthritis, the role of MSCs-derived EVs has never been reported in rheumatoid arthritis. This prompted us to compare the function of exosomes (Exos) and microparticles (MPs) isolated from MSCs and investigate their immunomodulatory function in arthritis.
Methods: MSCs-derived Exos and MPs were isolated by differential ultracentrifugation. Immunosuppressive effects of MPs or Exos were investigated on T and B lymphocytes in vitro and in the Delayed-Type Hypersensitivity (DTH) and Collagen-Induced Arthritis (CIA) models.
Results: Exos and MPs from MSCs inhibited T lymphocyte proliferation in a dose-dependent manner and decreased the percentage of CD4+ and CD8+ T cell subsets. Interestingly, Exos increased Treg cell populations while parental MSCs did not. Conversely, plasmablast differentiation was reduced to a similar extent by MSCs, Exos or MPs. IFN-γ priming of MSCs before vesicles isolation did not influence the immunomodulatory function of isolated Exos or MPs. In DTH, we observed a dose-dependent anti-inflammatory effect of MPs and Exos, while in the CIA model, Exos efficiently decreased clinical signs of inflammation. The beneficial effect of Exos was associated with fewer plasmablasts and more Breg-like cells in lymph nodes.
Conclusions: Both MSCs-derived MPs and Exos exerted an anti-inflammatory role on T and B lymphocytes independently of MSCs priming. However, Exos were more efficient in suppressing inflammation in vivo. Our work is the first demonstration of the therapeutic potential of MSCs-derived EVs in inflammatory arthritis.
Keywords: mesenchymal stem cells, extracellular vesicles, trophic factors, cell therapy, rheumatoid arthritis
 Global reach, higher impact
Global reach, higher impact