13.3
Impact Factor
Theranostics 2018; 8(17):4837-4855. doi:10.7150/thno.24512 This issue Cite
Research Paper
MRI and histological evaluation of pulsed focused ultrasound and microbubbles treatment effects in the brain
1. Frank Laboratory, Radiology and Imaging Sciences, Clinical Center, National Institutes of Health, Bethesda
2. Center for Neuroscience and Regenerative Medicine, Uniformed Services University of the Health Sciences, Bethesda
3. Molecular Imaging Laboratory, Department of Radiology, Howard University, Washington DC
4. National Institute of Biomedical Imaging and Bioengineering, National Institutes of Health, Bethesda
Abstract
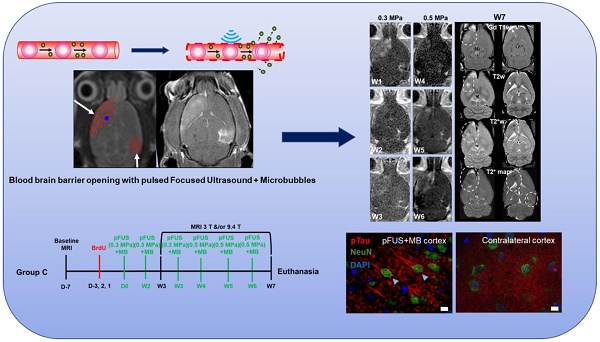
Magnetic resonance imaging (MRI)-guided pulsed focused ultrasound (pFUS) combined with microbubbles (MB) contrast agent infusion has been shown to transiently disrupt the blood-brain barrier (BBBD), increasing the delivery of neurotherapeutics to treat central nervous system (CNS) diseases. pFUS interaction with the intravascular MB results in acoustic cavitation forces passing through the neurovascular unit (NVU), inducing BBBD detected on contrast-enhanced MRI. Multiple pFUS+MB exposures in Alzheimer's disease (AD) models are being investigated as a method to clear amyloid plaques by activated microglia or infiltrating immune cells. Since it has been reported that pFUS+MB can induce a sterile inflammatory response (SIR) [1-5] in the rat, the goal of this study was to investigate the potential long-term effects of SIR in the brain following single and six weekly sonications by serial high-resolution MRI and pathology.
Methods: Female Sprague Dawley rats weighing 217±16.6 g prior to sonication received bromo-deoxyuridine (BrdU) to tag proliferating cells in the brain. pFUS was performed at 548 kHz, ultrasound burst 10 ms and initial peak negative pressure of 0.3 MPa (in water) for 120 s coupled with a slow infusion of ~460 µL/kg (5-8×107 MB) that started 30 s before and 30 s during sonication. Nine 2 mm focal regions in the left cortex and four regions over the right hippocampus were treated with pFUS+MB. Serial high-resolution brain MRIs at 3 T and 9.4 T were obtained following a single or during the course of six weekly pFUS+MB resulting in BBBD in the left cortex and the right hippocampus. Animals were monitored over 7 to 13 weeks and imaging results were compared to histology.
Results: Fewer than half of the rats receiving a single pFUS+MB exposure displayed hypointense voxels on T2*-weighted (w) MRI at week 7 or 13 in the cortex or hippocampus without differences compared to the contralateral side on histograms of T2* maps. Single sonicated rats had evidence of limited microglia activation on pathology compared to the contralateral hemisphere. Six weekly pFUS+MB treatments resulted in pathological changes on T2*w images with multiple hypointense regions, cortical atrophy, along with 50% of rats having persistent BBBD and astrogliosis by MRI. Pathologic analysis of the multiple sonicated animals demonstrated the presence of metallophagocytic Prussian blue-positive cells in the parenchyma with significantly (p<0.05) increased areas of activated astrocytes and microglia, and high numbers of systemic infiltrating CD68+ macrophages along with BrdU+ cells compared to contralateral brain. In addition, multiple treatments caused an increase in the number of hyperphosphorylated Tau (pTau)-positive neurons containing neurofibrillary tangles (NFT) in the sonicated cortex but not in the hippocampus when compared to contralateral brain, which was confirmed by Western blot (WB) (p<0.04).
Conclusions: The repeated SIR following multiple pFUS+MB treatments could contribute to changes on MR imaging including persistent BBBD, cortical atrophy, and hypointense voxels on T2w and T2*w images consistent with pathological injury. Moreover, areas of astrogliosis, activated microglia, along with higher numbers of CD68+ infiltrating macrophages and BrdU+ cells were detected in multiple sonicated areas of the cortex and hippocampus. Elevations in pTau and NFT were detected in neurons of the multiple sonicated cortex. Minimal changes on MRI and histology were observed in single pFUS+MB-treated rats at 7 and 13 weeks post sonication. In comparison, animals that received 6 weekly sonications demonstrated evidence on MRI and histology of vascular damage, inflammation and neurodegeneration associated with the NVU commonly observed in trauma. Further investigation is recommended of the long-term effects of multiple pFUS+MB in clinical trials.
Keywords: pulsed focused ultrasound, microbubbles, sterile inflammation, blood-brain barrier, hyperphosphorylated Tau
 Global reach, higher impact
Global reach, higher impact