Impact Factor
Theranostics 2019; 9(7):2071-2083. doi:10.7150/thno.29581 This issue Cite
Research Paper
Pharmacologic modulation of nasal epithelium augments neural stem cell targeting of glioblastoma
1. The Brain Tumor Center, University of Chicago, Chicago, IL 60637, USA
2. Department of Neurological Surgery, Northwestern University at Chicago, 676 N. Saint Clair, Suite 2210, Chicago, IL 60611 USA
3. Department of Neurological Surgery, University of California San Francisco, 505 Parnassus Avenue, Rm M779, San Francisco, CA 94143 USA
4. Department of Radiology, Northwestern University at Chicago, 737 North Michigan Avenue, Suite 1600, Chicago, IL 60611 USA
Abstract
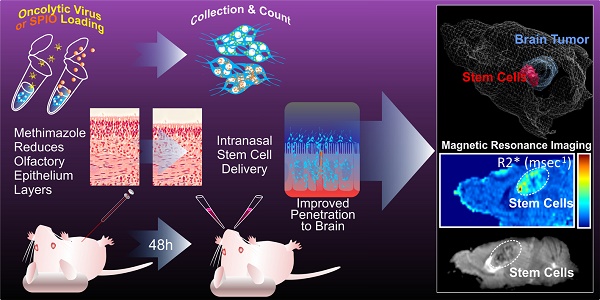
Glioblastoma (GBM) remains the most lethal and untreatable central nervous system malignancy. The challenges to devise novel and effective anti-tumor therapies include difficulty in locating the precise tumor border for complete surgical resection, and rapid regrowth of residual tumor tissue after standard treatment. Repeatable and non-invasive intranasal application of neural stem cells (NSCs) was recently shown to enable clinically relevant delivery of therapy to tumors. Treatment with chemotactic NSCs demonstrated significant survival benefits when coupled with radiation and oncolytic virotherapy in preclinical models of GBM. In order to further augment the clinical applicability of this novel therapeutic platform, we postulate that the FDA-approved compound, methimazole (MT), can be safely utilized to delay the nasal clearance and improve the ability of NSCs to penetrate the olfactory epithelium for robust in vivo brain tumor targeting and therapeutic actions. METHODS: To examine the role of reversible reduction of the olfactory epithelial barrier in non-invasive intranasal delivery, we explored the unique pharmacologic effect of MT at a single dosage regimen. In our proof-of-concept studies, quantitative magnetic resonance imaging (MRI), immunocytochemistry, and survival analysis were performed on glioma-bearing mice treated with a single dose of MT prior to intranasal anti-GBM therapy using an oncolytic virus (OV)-loaded NSCs. RESULTS: Based on histology and in vivo imaging, we found that disrupting the olfactory epithelium with MT effectively delays clearance and allows NSCs to persist in the nasal cavity for at least 24 h. MT pretreatment amplified the migration of NSCs to the tumor. The therapeutic advantage of this enhancement was quantitatively validated by tissue analysis and MRI tracking of NSCs loaded with superparamagnetic iron oxide nanoparticles (SPIOs) in live animals. Moreover, we observed significant survival benefits in GBM-bearing mice treated with intranasal delivery of oncolytic virus-loaded NSCs following MT injection. Conclusion: Our work identified a novel pharmacologic strategy to accelerate the clinical application of the non-invasive NSCs-based therapeutic platform to tackle aggressive brain tumors.
Keywords: neural stem cells, intranasal delivery, glioblastoma, clearance, barrier
 Global reach, higher impact
Global reach, higher impact