13.3
Impact Factor
Theranostics 2019; 9(19):5720-5730. doi:10.7150/thno.36639 This issue Cite
Research Paper
Glyoxalase 1 Prevents Chronic Hyperglycemia Induced Heart-Explant Derived Cell Dysfunction
1. University of Ottawa Heart Institute, Division of Cardiology, Department of Medicine, University of Ottawa, Ottawa, Canada K1Y4W7
2. Department of Biochemistry, Microbiology and Immunology, Faculty of Medicine, University of Ottawa, Ottawa, Canada K1H8M5
3. Department of Cellular and Molecular Medicine, Faculty of Medicine, University of Ottawa, Ottawa, Canada K1H8M5
Abstract
Decades of work have shown that diabetes increases the risk of heart disease and worsens clinical outcomes after myocardial infarction. Because diabetes is an absolute contraindication to heart transplant, cell therapy is increasingly being explored as a means of improving heart function for these patients with very few other options. Given that hyperglycemia promotes the generation of toxic metabolites, the influence of the key detoxification enzyme glyoxalase 1 (Glo1) on chronic hyperglycemia induced heart explant-derived cell (EDC) dysfunction was investigated.
Methods: EDCs were cultured from wild type C57Bl/6 or Glo1 over-expressing transgenic mice 2 months after treatment with the pancreatic beta cell toxin streptozotocin or vehicle. The effects of Glo1 overexpression was evaluated using in vitro and in vivo models of myocardial ischemia.
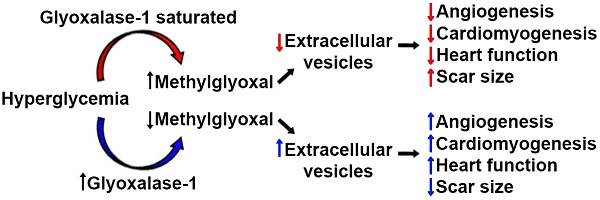
Results: Chronic hyperglycemia reduced overall culture yields and increased the reactive dicarbonyl cell burden within EDCs. These intrinsic cell changes reduced the angiogenic potential and production of pro-healing exosomes while promoting senescence and slowing proliferation. Compared to intra-myocardial injection of normoglycemic cells, chronic hyperglycemia attenuated cell-mediated improvements in myocardial function and reduced the ability of transplanted cells to promote new blood vessel and cardiomyocyte growth. In contrast, Glo1 overexpression decreased oxidative damage while restoring both cell culture yields and EDC-mediated repair of ischemic myocardium. The latter was associated with enhanced production of pro-healing extracellular vesicles by Glo1 cells without altering the pro-healing microRNA cargo within.
Conclusions: Chronic hyperglycemia decreases the regenerative performance of EDCs. Overexpression of Glo1 reduces dicarbonyl stress and prevents chronic hyperglycemia-induced dysfunction by rejuvenating the production of pro-healing extracellular vesicles.
Keywords: cardiac stem cells, diabetes, extracellular vesicles, hyperglycemia, heart failure, myocardial infarction, oxidative stress, reactive dicarbonyls
 Global reach, higher impact
Global reach, higher impact