Impact Factor
Theranostics 2019; 9(21):6284-6299. doi:10.7150/thno.35892 This issue Cite
Research Paper
Acoustic feedback enables safe and reliable carboplatin delivery across the blood-brain barrier with a clinical focused ultrasound system and improves survival in a rat glioma model
1. Department of Radiology, Brigham and Women's Hospital, Harvard Medical School, Boston, MA
2. Department of Medicine, Massachusetts General Hospital, Harvard Medical School, Boston, MA
3. Department of Neurosurgery, Brigham and Women's Hospital, Harvard Medical School, Boston, MA
4. Electrical Engineering, Boston University, Boston, MA
5. Department of Medical Oncology, Dana-Farber Cancer Institute; Department of Medicine, Brigham and Women's Hospital; Harvard Medical School, Boston, MA
Abstract
The blood-brain barrier (BBB) restricts delivery of most chemotherapy agents to brain tumors. Here, we investigated a clinical focused ultrasound (FUS) device to disrupt the BBB in rats and enhance carboplatin delivery to the brain using the F98 glioma model.
Methods: In each rat, 2-3 volumetric sonications (5 ms bursts at 1.1 Hz for 75s) targeted 18-27 locations in one hemisphere. Sonication was combined with Definity microbubbles (10 µl/kg) and followed by intravenous carboplatin (50 mg/kg). Closed-loop feedback control was performed based on acoustic emissions analysis.
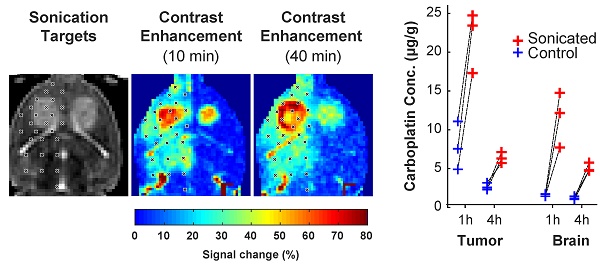
Results: Safety and reliability were established in healthy rats after three sessions with carboplatin; BBB disruption was induced in every target without significant damage evident in MRI or histology. In tumor-bearing rats, concentrations of MRI contrast agent (Gadavist) were 1.7 and 3.3 times higher in the tumor center and margin, respectively, than non-sonicated tumors (P<0.001). Tissue-to-plasma ratios of intact carboplatin concentrations were increased by 7.3 and 2.9 times in brain and tumor respectively, at one hour after FUS and 4.2 and 2.4 times at four hours. Tumor volume doubling time in rats receiving FUS and carboplatin increased by 96% and 126% compared to rats that received carboplatin alone and non-sonicated controls, respectively (P<0.05); corresponding increases in median survival were 48% and 66% (P<0.01).
Conclusion: Overall, this work demonstrates that actively-controlled BBB disruption with a clinical device can enhance carboplatin delivery without neurotoxicity at level that reduces tumor growth and improves survival in an aggressive and infiltrative rat glioma model.
Keywords: Ultrasound, blood-brain barrier, brain tumor, chemotherapy
 Global reach, higher impact
Global reach, higher impact