Impact Factor
Theranostics 2020; 10(6):2773-2790. doi:10.7150/thno.39072 This issue Cite
Research Paper
Inflammatory extracellular vesicles prompt heart dysfunction via TRL4-dependent NF-κB activation
1. Laboratory for Cardiovascular Theranostics, Cardiocentro Ticino Foundation, Lugano, Switzerland
2. Laboratory of Cellular and Molecular Cardiology, Cardiocentro Ticino Foundation, Lugano, Switzerland
3. Dept. Cœur-Vaisseaux, Centre Hospitalier Universitaire Vaudois, Lausanne, Switzerland
4. Department of Health Sciences of the University of Milan, Milan, Italy
5. Cell and Biomedical Technologies Unit Cardiocentro Ticino Foundation, Lugano, Switzerland
6. Department of Cardiology, Cardiocentro Ticino Foundation, Lugano, Switzerland
7. Department of Cardiovascular Surgery, Inselspital, Bern University Hospital, Bern, Switzerland
8. Faculty of Biomedical Sciences, Università della Svizzera Italiana, Lugano, Switzerland
Abstract
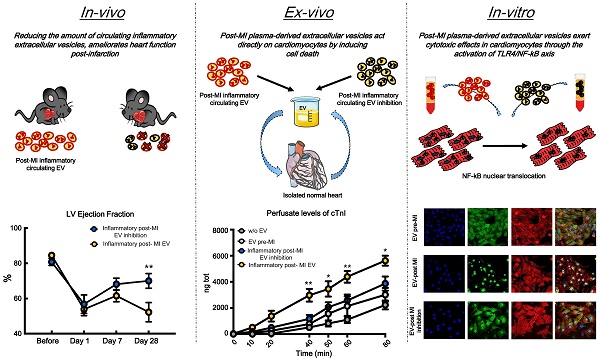
Background: After myocardial infarction, necrotic cardiomyocytes release damage-associated proteins that stimulate innate immune pathways and macrophage tissue infiltration, which drives inflammation and myocardial remodeling. Circulating inflammatory extracellular vesicles play a crucial role in the acute and chronic phases of ischemia, in terms of inflammatory progression. In this study, we hypothesize that the paracrine effect mediated by these vesicles induces direct cytotoxicity in cardiomyocytes. Thus, we examined whether reducing the generation of inflammatory vesicles within the first few hours after the ischemic event ameliorates cardiac outcome at short and long time points.
Methods: Myocardial infarction was induced in rats that were previously injected intraperitoneally with a chemical inhibitor of extracellular-vesicle biogenesis. Heart global function was assessed by echocardiography performed at 7, 14 and 28 days after MI. Cardiac outcome was also evaluated by hemodynamic analysis at sacrifice. Cytotoxic effects of circulating EV were evaluated ex-vivo in a Langendorff, system by measuring the level of cardiac troponin I (cTnI) in the perfusate. Mechanisms undergoing cytotoxic effects of EV derived from pro-inflammatory macrophages (M1) were studied in-vitro in primary rat neonatal cardiomyocytes.
Results: Inflammatory response following myocardial infarction dramatically increased the number of circulating extracellular vesicles carrying alarmins such as IL-1α, IL-1β and Rantes. Reducing the boost in inflammatory vesicles during the acute phase of ischemia resulted in preserved left ventricular ejection fraction in vivo. Hemodynamic analysis confirmed functional recovery by displaying higher velocity of left ventricular relaxation and improved contractility. When added to the perfusate of isolated hearts, post-infarction circulating vesicles induced significantly more cell death in adult cardiomyocytes, as assessed by cTnI release, comparing to circulating vesicles isolated from healthy (non-infarcted) rats. In vitro inflammatory extracellular vesicles induce cell death by driving nuclear translocation of NF-κB into nuclei of cardiomyocytes.
Conclusion: Our data suggest that targeting circulating extracellular vesicles during the acute phase of myocardial infarction may offer an effective therapeutic approach to preserve function of ischemic heart.
Keywords: myocardial infarction, inflammatory extracellular vesicles, macrophages, TLR4 axis
 Global reach, higher impact
Global reach, higher impact