Impact Factor
Theranostics 2020; 10(14):6372-6383. doi:10.7150/thno.46833 This issue Cite
Research Paper
Risk factors for adverse clinical outcomes with COVID-19 in China: a multicenter, retrospective, observational study
1. Department of Medical Imaging, Jinling Hospital, Medical School of Nanjing University, Nanjing, Jiangsu, 210002, China.
2. Department of Medical Imaging, Xiaogan Central Hospital of Wuhan University of Science and Technology, Xiaogan, Hubei, China.
3. Huanggang Central Hospital, No. 11, Kaopeng Road, Huangzhou District, Huanggang, Hubei, China.
4. Department of Medical Imaging, Shandong Provincial Hospital Affiliated to Shandong First Medical University, Jinan, Shandong, China.
5. Department of Radiology, the Affiliated Hospital of Xuzhou Medical University, Xuzhou, Jiangsu, China.
6. Institute of Medical Imaging and Digital Medicine, Xuzhou Medical University, Xuzhou, Jiangsu, China.
7. Department of Radiology, Xiangyang Central Hospital, Affiliated Hospital of Hubei University of Arts and Science, Xiangyang, Hubei, China.
8. Department of Medical Imaging, the Affiliated Anqing Hospital of Anhui Medical University, Anqing, Anhui, China.
9. Departments of Infectious Disease & Department of Medical Imaging, Wenzhou Central Hospital, Wenzhou, Zhejiang, China.
10. Department of Radiology, Hainan General Hospital, Haikou, Hainan, China.
11. Department of Medical Imaging, Jingzhou Central Hospital, The Second Clinical Medical College, Yangtze University, Jingzhou, Hubei, China.
12. Department of Medical Imaging, The Second Affiliated Hospital and Yuying Children's Hospital of Wenzhou Medical University, Wenzhou, Zhejiang, PR China.
13. Department of Medical Imaging, Guizhou Provincial People's Hospital, Guiyang, China.
14. Department of Medical Imaging, Taihe Hospital, Hubei University of Medicine, Shiyan, Hubei, China.
15. Department of Radiology, General Hospital of the Yangtze River Shipping, Wuhan, Hubei, China.
16. Department of Radiology, Yichang Central People's Hospital, Yichang, Hubei, China.
17. Department of Radiology, The First Hospital of China Medical University, Shenyang, Liaoning, China.
#These authors contributed equally to this work.
Abstract
Background: The risk factors for adverse events of Coronavirus Disease-19 (COVID-19) have not been well described. We aimed to explore the predictive value of clinical, laboratory and CT imaging characteristics on admission for short-term outcomes of COVID-19 patients.
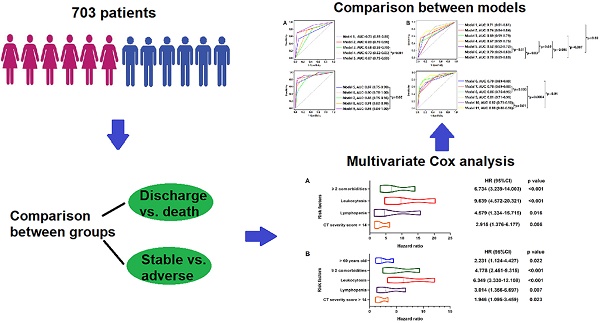
Methods: This multicenter, retrospective, observation study enrolled 703 laboratory-confirmed COVID-19 patients admitted to 16 tertiary hospitals from 8 provinces in China between January 10, 2020 and March 13, 2020. Demographic, clinical, laboratory data, CT imaging findings on admission and clinical outcomes were collected and compared. The primary endpoint was in-hospital death, the secondary endpoints were composite clinical adverse outcomes including in-hospital death, admission to intensive care unit (ICU) and requiring invasive mechanical ventilation support (IMV). Multivariable Cox regression, Kaplan-Meier plots and log-rank test were used to explore risk factors related to in-hospital death and in-hospital adverse outcomes.
Results: Of 703 patients, 55 (8%) developed adverse outcomes (including 33 deceased), 648 (92%) discharged without any adverse outcome. Multivariable regression analysis showed risk factors associated with in-hospital death included ≥ 2 comorbidities (hazard ratio [HR], 6.734; 95% CI; 3.239-14.003, p < 0.001), leukocytosis (HR, 9.639; 95% CI, 4.572-20.321, p < 0.001), lymphopenia (HR, 4.579; 95% CI, 1.334-15.715, p = 0.016) and CT severity score > 14 (HR, 2.915; 95% CI, 1.376-6.177, p = 0.005) on admission, while older age (HR, 2.231; 95% CI, 1.124-4.427, p = 0.022), ≥ 2 comorbidities (HR, 4.778; 95% CI; 2.451-9.315, p < 0.001), leukocytosis (HR, 6.349; 95% CI; 3.330-12.108, p < 0.001), lymphopenia (HR, 3.014; 95% CI; 1.356-6.697, p = 0.007) and CT severity score > 14 (HR, 1.946; 95% CI; 1.095-3.459, p = 0.023) were associated with increased odds of composite adverse outcomes.
Conclusion: The risk factors of older age, multiple comorbidities, leukocytosis, lymphopenia and higher CT severity score could help clinicians identify patients with potential adverse events.
Keywords: COVID-19, Coronavirus, Pneumonia, Risk factor, Mortality
 Global reach, higher impact
Global reach, higher impact