13.3
Impact Factor
Theranostics 2021; 11(5):2424-2441. doi:10.7150/thno.46873 This issue Cite
Research Paper
Inhibitory effect of PPARγ on NLRP3 inflammasome activation
1. Institute of Clinical Medicine, College of Medicine, National Cheng Kung University, Tainan, Taiwan, ROC.
2. Department of Medical Laboratory Science and Biotechnology, College of Medicine, National Cheng Kung University, Tainan, Taiwan, ROC.
3. Department of Family Medicine, National Cheng Kung University Hospital, College of Medicine, National Cheng Kung University, Tainan, Taiwan, ROC.
4. Institute of Gerontology, College of Medicine, National Cheng Kung University, Tainan, Taiwan, ROC.
5. Department of Surgery, National Cheng Kung University Hospital, College of Medicine, National Cheng Kung University, Tainan, Taiwan, ROC.
6. Center for Clinical Medicine Research, National Cheng Kung University Hospital, College of Medicine, National Cheng Kung University, Tainan, Taiwan, ROC.
Abstract
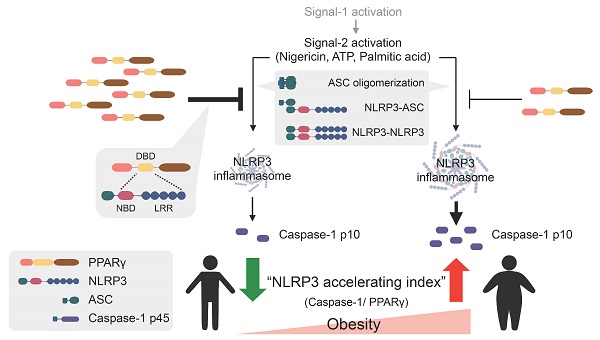
Rationale: Stimulation of the NLRP3 inflammasome by metabolic byproducts is known to result in inflammatory responses and metabolic diseases. However, how the host controls aberrant NLRP3 inflammasome activation remains unclear. PPARγ, a known regulator of energy metabolism, plays an anti-inflammatory role through the inhibition of NF-κB activation and additionally attenuates NLRP3-dependent IL-1β and IL-18 production. Therefore, we hypothesized that PPARγ serves as an endogenous modulator that attenuates NLRP3 inflammasome activation in macrophages.
Methods: Mouse peritoneal macrophages with exposure to a PPARγ agonist at different stages and the NLRP3 inflammasome-reconstituted system in HEK293T cells were used to investigate the additional anti-inflammatory effect of PPARγ on NLRP3 inflammasome regulation. Circulating mononuclear cells of obese patients with weight-loss surgery were used to identify the in vivo correlation between PPARγ and the NLRP3 inflammasome.
Results: Exposure to the PPARγ agonist, rosiglitazone, during the second signal of NLRP3 inflammasome activation attenuated caspase-1 and IL-1β maturation. Moreover, PPARγ interfered with NLRP3 inflammasome formation by decreasing NLRP3-ASC and NLRP3-NLRP3 interactions as well as NLRP3-dependent ASC oligomerization, which is mediated through interaction between the PPARγ DNA-binding domain and the nucleotide-binding and leucine-rich repeat domains of NLRP3. Furthermore, PPARγ was required to limit metabolic damage-associated molecular pattern-induced NLRP3 inflammasome activation in mouse macrophages. Finally, the mature caspase-1/PPARγ ratio was reduced in circulating mononuclear cells of obese patients after weight-loss surgery, which we define as an “NLRP3 accelerating index”.
Conclusions: These results revealed an additional anti-inflammatory role for PPARγ in suppressing NLRP3 inflammasome activation through interaction with NLRP3. Thus, our study highlights that PPARγ agonism may be a therapeutic option for targeting NLRP3-related metabolic diseases.
Keywords: NLRP3 inflammasome/ macrophages/ obesity/ PPARγ/ rosiglitazone
 Global reach, higher impact
Global reach, higher impact