13.3
Impact Factor
Theranostics 2021; 11(17):8129-8142. doi:10.7150/thno.62069 This issue Cite
Research Paper
Mesenchymal stem cell-derived extracellular vesicles ameliorate Alzheimer's disease-like phenotypes in a preclinical mouse model
1. Department of Biomedical Sciences, Florida State University College of Medicine, Tallahassee, FL 32306, USA
2. Department of Chemical and Biomedical Engineering, Florida A&M University and Florida State University College of Engineering, Tallahassee, FL 32306, USA
3. The National High Magnetic Field Laboratory, Florida State University, Tallahassee, Florida 32310, USA
4. Department of Neuroscience, Florida State University College of Psychology, Tallahassee, FL 32306, USA
Abstract
Alzheimer's disease (AD) is an irreversible neurodegenerative disorder that affects more than 44 million people worldwide. Despite the high disease burden, there is no effective treatment for people suffering from AD. Mesenchymal stem cells (MSCs) are multipotent stromal cells that have been widely studied due to their therapeutic potential. However, administration of cells has been found to have a multitude of limitations. Recently, extracellular vesicles (EVs) derived from MSCs have been studied as a therapeutic candidate, as they exhibit similar immunoprotective and immunomodulatory abilities as the host human MSCs.
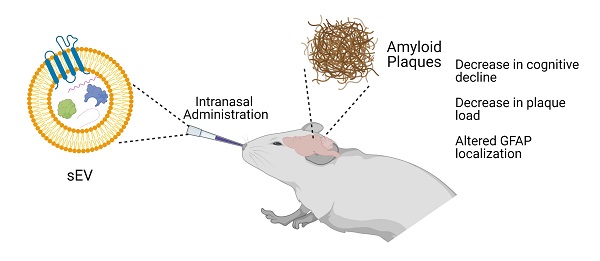
Methods: To test the potential therapeutic effects of MSC EVs, human bone-marrow derived MSCs were grown in three-dimensional (3D) cell culture, and small EVs were harvested using differential ultracentrifugation. These small EVs were given to non-transgenic (NT) or 5XFAD (5 familial Alzheimer's disease mutations) mice intranasally (IN) every 4 days for 4 months. The mice were then required to perform a variety of behavioral assays to measure changes in learning and memory. Afterwards, immunohistochemistry was performed on brain slices to measure amyloid beta (Aβ) and glial fibrillary acidic protein (GFAP) levels.
Results: The data revealed that 5XFAD mice that received hMSC-EV treatment behaved significantly better in cognitive tests than saline treated 5XFAD mice, with no significant change between EV-treated 5XFAD mice and NT mice. Additionally, we found lower Aβ plaque load in the hippocampus of the EV-treated mice. Finally, less colocalization between GFAP and Aβ plaques was found in the brain of EV-treated mice compared to saline.
Conclusions: Taken together, these data suggest that IN administration of MSC-derived EVs can slow down AD pathogenesis.
Keywords: Alzheimer's disease, extracellular vesicles, exosomes, microvesicles, mesenchymal stem cells
 Global reach, higher impact
Global reach, higher impact