13.3
Impact Factor
Theranostics 2023; 13(6):1759-1773. doi:10.7150/thno.81336 This issue Cite
Research Paper
CSF2RB overexpression promotes the protective effects of mesenchymal stromal cells against ischemic heart injury
1. Department of Cardiology, Xijing Hospital, Fourth Military Medical University, Xi'an 710032, China.
2. School of Public Management, Northwest University, Xi'an 710127, China.
3. Department of Toxicology, The Ministry of Education Key Lab of Hazard Assessment and Control in Special Operational Environment, Shanxi Key Lab of Free Radical Biology and Medicine, School of Public Health, The Fourth Military Medical University, Xi'an 710032, China.
4. Department of Occupational and Environmental Health and the Ministry of Education Key Lab of Hazard Assessment and Control in Special Operational Environment, School of Public Health, Fourth Military Medical University, Xi'an 710032, China.
5. Center for Translational Medicine, Temple University, Philadelphia, PA 19140, USA.
6. Key Laboratory of Aerospace Medicine of the Ministry of Education, School of Aerospace Medicine, Fourth Military Medical University, Xi'an 710032, China.
#Tingting Qi, Xiaoming Xu, and Yongzhen Guo contributed equally to this work.
Abstract
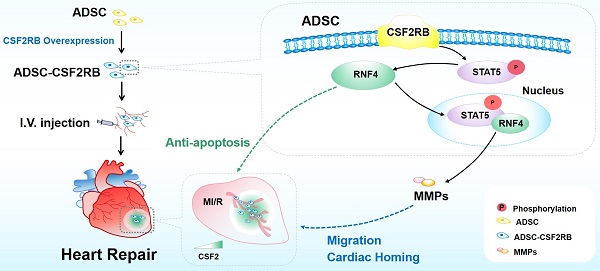
Aims: The invasive intramyocardial injection of mesenchymal stromal cells (MSCs) allows for limited repeat injections and shows poor therapeutic efficacy against ischemic heart failure. Intravenous injection is an alternative method because this route allows for repeated, noninvasive, and easy delivery. However, the lack of targeting of MSCs hinders the ability of these cells to accumulate in the ischemic area after intravenous injections. We investigated whether and how the overexpression of colony-stimulating factor 2 receptor beta subunit (CSF2RB) may regulate the cardiac homing of MSCs and their cardioprotective effects against ischemic heart failure.
Methods and Results: Adult mice were subjected to myocardial ischemia/reperfusion (MI/R) or sham operations. We observed significantly higher CSF2 protein expression and secretion by the ischemic heart from 1 day to 2 weeks after MI/R. Mouse adipose tissue-derived MSCs (ADSCs) were infected with adenovirus harboring CSF2RB or control adenovirus. Enhanced green fluorescent protein (EGFP)-labeled ADSCs were intravenously injected into MI/R mice every three days for a total of 7 times. Compared with ADSCs infected with control adenovirus, intravenously delivered ADSCs overexpressing CSF2RB exhibited markedly increased cardiac homing. Histological analysis revealed that CSF2RB overexpression significantly enhanced the ADSC-mediated proangiogenic, antiapoptotic, and antifibrotic effects. More importantly, ADSCs overexpressing CSF2RB significantly increased the left ventricular ejection fraction and cardiac contractility/relaxation in MI/R mice. In vitro experiments demonstrated that CSF2RB overexpression increases the migratory capacity and reduces the hypoxia/reoxygenation-induced apoptosis of ADSCs. We identified STAT5 phosphorylation as the key mechanism underlying the effects of CSF2RB on promoting ADSC migration and inhibiting ADSC apoptosis. RNA sequencing followed by cause-effect analysis revealed that CSF2RB overexpression increases the expression of the ubiquitin ligase RNF4. Coimmunoprecipitation and coimmunostaining experiments showed that RNF4 binds to phosphorylated STAT5. RNF4 knockdown reduced STAT5 phosphorylation as well as the antiapoptotic and promigratory actions of ADSCs overexpressing CSF2RB.
Conclusions: We demonstrate for the first time that CSF2RB overexpression optimizes the efficacy of intravenously delivered MSCs in the treatment of ischemic heart injury by increasing the response of the MSCs to a CSF2 gradient and CSF2RB-dependent STAT5/RNF4 activation.
Keywords: CSF2RB, ischemic heart injury, mesenchymal stromal cells, RNF4, STAT5
 Global reach, higher impact
Global reach, higher impact