Impact Factor
Theranostics 2020; 10(2):462-483. doi:10.7150/thno.37593 This issue Cite
Review
Micro/nano-bubble-assisted ultrasound to enhance the EPR effect and potential theranostic applications
1. School of Biomedical Engineering and Informatics, Nanjing Medical University, Nanjing, 211166, P. R. China.
2. State Key Laboratory of Bioelectronics, Jiangsu Key Laboratory for Biomaterials and Devices, School of Biological Science and Medical Engineering, Southeast University, Nanjing 210096, P. R. China.
3. West Anhui University, Lu'an, P.R. China
4. Anhui Engineering Laboratory for Conservation and Sustainable Utilization of Traditional Chinese Medicine Resources, P. R. China.
*These authors contributed equally to this work.
Abstract
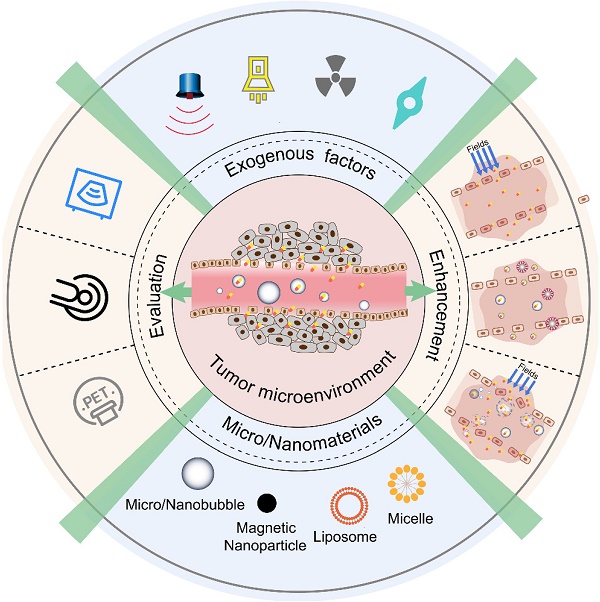
Drug delivery for tumor theranostics involves the extensive use of the enhanced permeability and retention (EPR) effect. Previously, various types of nanomedicines have been demonstrated to accumulate in solid tumors via the EPR effect. However, EPR is a highly variable phenomenon because of tumor heterogeneity, resulting in low drug delivery efficacy in clinical trials. Because ultrasonication using micro/nanobubbles as contrast agents can disrupt blood vessels and enhance the specific delivery of drugs, it is an effective approach to improve the EPR effect for the passive targeting of tumors. In this review, the basic thermal effect, acoustic streaming, and cavitation mechanisms of ultrasound, which are characteristics that can be utilized to enhance the EPR effect, are briefly introduced. Second, micro/nanobubble-enhanced ultrasound imaging is discussed to understand the validity and variability of the EPR effect. Third, because the tumor microenvironment is complicated owing to elevated interstitial fluid pressure and the deregulated extracellular matrix components, which may be unfavorable for the EPR effect, few new trends in smart bubble drug delivery systems, which may improve the accuracy of EPR-mediated passive drug targeting, are summarized. Finally, the challenging and major concerns that should be considered in the next generation of micro/nanobubble-contrast-enhanced ultrasound theranostics for EPR-mediated passive drug targeting are also discussed.
Keywords: EPR effect, ultrasound, micro/nanobubbles, controlled drug delivery, tumor theranostics
 Global reach, higher impact
Global reach, higher impact