Impact Factor
Theranostics 2019; 9(18):5374-5385. doi:10.7150/thno.34149 This issue Cite
Research Paper
A radiomics approach based on support vector machine using MR images for preoperative lymph node status evaluation in intrahepatic cholangiocarcinoma
1. Sir Run Run Shaw Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, China
2. Institute of Translational Medicine, Zhejiang University, Hangzhou, Zhejiang, China
3. College of Biomedical Engineering &Instrument Science, Zhejiang University, Hangzhou, Zhejiang, China
4. Department of Radiology, the First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, China
5. Department of Radiology, the First Hospital of Ninghai County Medical Centre, Ningbo, Zhejiang, China
6. Department of Radiation Oncology, Stanford University School of Medicine, Stanford, California, USA
7. Department of Radiation Oncology, Duke University Medical Center, Durham, USA
8. Department of Hepatobiliary and Pancreatic Surgery, the First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, China
9. Engineering Research Center of Cognitive Healthcare of Zhejiang Province
*: Both authors contribute equally.
Abstract
Purpose: Accurate lymph node (LN) status evaluation for intrahepatic cholangiocarcinoma (ICC) patients is essential for surgical planning. This study aimed to develop and validate a prediction model for preoperative LN status evaluation in ICC patients.
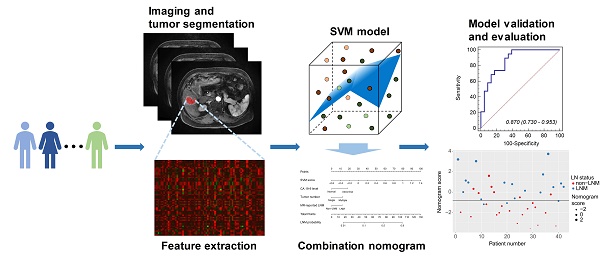
Methods and Materials: A group of 106 ICC patients, who were diagnosed between April 2011 and February 2016, was used for prediction model training. Image features were extracted from T1-weighted contrast-enhanced MR images. A support vector machine (SVM) model was built by using the most LN status-related features, which were selected using the maximum relevance minimum redundancy (mRMR) algorithm. The mRMR method ranked each feature according to its relevance to the LN status and redundancy with other features. An SVM score was calculated for each patient to reflect the LN metastasis (LNM) probability from the SVM model. Finally, a combination nomogram was constructed by incorporating the SVM score and clinical features. An independent group of 42 patients who were diagnosed from March 2016 to November 2017 was used to validate the prediction models. The model performances were evaluated on discrimination, calibration, and clinical utility.
Results: The SVM model was constructed based on five selected image features. Significant differences were found between patients with LNM and non-LNM in SVM scores in both groups (the training group: 0.5466 (interquartile range (IQR), 0.4059-0.6985) vs. 0.3226 (IQR, 0.0527-0.4659), P<0.0001; the validation group: 0.5831 (IQR, 0.3641-0.8162) vs. 0.3101 (IQR, 0.1029-0.4661), P=0.0015). The combination nomogram based on the SVM score, the CA 19-9 level, and the MR-reported LNM factor showed better discrimination in separating patients with LNM and non-LNM, comparing to the SVM model alone (AUC: the training group: 0.842 vs. 0.788; the validation group: 0.870 vs. 0.787). Favorable clinical utility was observed using the decision curve analysis for the nomogram.
Conclusion: The nomogram, incorporating the SVM score, CA 19-9 level and the MR-reported LNM factor, provided an individualized LN status evaluation and helped clinicians guide the surgical decisions.
Keywords: Radiomics, intrahepatic cholangiocarcinoma, lymph node metastasis
 Global reach, higher impact
Global reach, higher impact