13.3
Impact Factor
Theranostics 2020; 10(14):6082-6094. doi:10.7150/thno.44584 This issue Cite
Research Paper
Immunohistochemical PSMA expression patterns of primary prostate cancer tissue are associated with the detection rate of biochemical recurrence with 68Ga-PSMA-11-PET
1. Department of Nuclear Medicine, University Hospital Zürich, University of Zürich, Zurich, Switzerland
2. Department of Pathology and Molecular Pathology, University Hospital Zurich, University of Zurich, Zurich, Switzerland.
3. Department of Interventional and Diagnostic Radiology, University Hospital Zurich, University of Zurich, Zurich, Switzerland
4. Department of Urology, University Hospital Zürich, University of Zurich, Zurich, Switzerland
5. Department of Nuclear Medicine, Kantonsspital Baden, Baden, Switzerland
*contributed equally to this work
#contributed equally to this work
Abstract
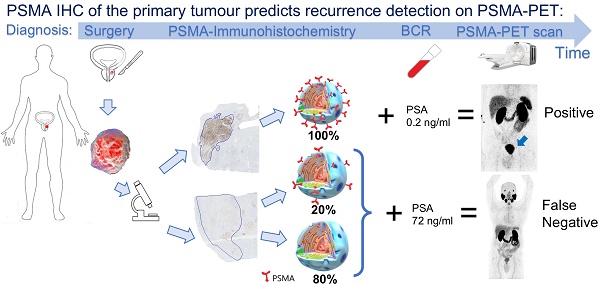
Prostate-specific membrane antigen (PSMA) targeted PET has a high detection rate for biochemical recurrence (BCR) of prostate cancer (PCa). Nevertheless, even at high prostate-specific antigen (PSA) levels (> 3 ng/ml), a relevant number of PSMA-PET scans are negative, mainly due to PSMA-negative PCa. Our objective was to investigate whether PSMA-expression patterns of the primary tumour on immunohistochemistry (IHC) are associated with PSMA-PET detection rate of recurrent PCa.
Methods: Retrospective institutional review board approved single-centre analysis of patients who had undergone 68Ga-PSMA-11-PET for BCR after radical prostatectomy (RPE) between 04/2016 and 07/2019, with tumour specimens available for PSMA-IHC. Clinical information (age, PSA-level, ongoing androgen deprivation therapy (ADT), Gleason score) and PSMA-IHC of the primary tumour were collected and their relationship to results from PSMA-PET (positive/negative) was investigated using a multiple logistic regression analysis.
Results: 120 PSMA-PET scans in 74 patients were available for this analysis. Overall detection rate was 62% (74/120 scans), with a mean PSA value at scan time of 0.99 ng/ml (IQR 0.32-4.27). Of the clinical factors, only PSA-level and ADT were associated with PSMA-PET positivity. The percentage of PSMA-negative tumour area on IHC (PSMA%neg) had a significant association to PSMA-PET negativity (OR = 2.88, p < 0.001), while membranous PSMA-expression showed no association (p = 0.73). The positive predictive value of PSMA%neg ≥ 50% for a negative PSMA-PET was 85% (13/11) and for a PSMA%neg of 80% or more, 100% (9/9).
Conclusions: PSMA-negative tumour area on IHC exhibited the strongest association with negative PSMA-PET scans, beside PSA-level and ADT. Even at very high PSA levels, PSMA-PET scans were negative in most of the patients with PSMA%neg ≥ 50%.
Keywords: immunohistochemistry, PSMA-negative prostate cancer, PSMA PET, PSMA staining, restaging
 Global reach, higher impact
Global reach, higher impact